Oh, Sierra. 😣
Our 13 year old daughter recently had a tonsillectomy at Children’s Hospital of Wisconsin in Milwaukee. We are in the middle of recovery at this point, but, I thought it would be a good idea to share about our experience thus far. That way you can know what to expect when your teenager has a tonsillectomy.
Let me preface this blog by saying that there’s a couple gross pictures ahead, so: reader beware. Y’all know how much I love to share about my parenting experiences, so hopefully if you ever have to go through a teenage tonsillectomy with your own kids, you’ll know what to expect and know that you’re not alone.
What to Expect When Your Teenager Has a Tonsillectomy
This surgery has honestly been a long time coming. Sierra has had strep throat so many times over the years that I’ve honestly lost count; it seems like she has been complaining about having a sore throat since she could talk. Earlier this month she had yet another sore throat and that was when I noticed a small ball of off-white colored “stuff” in her throat. Her breath was horrendous, no matter how well she brushed her teeth she had breath that smelled so bad it would make me gag.
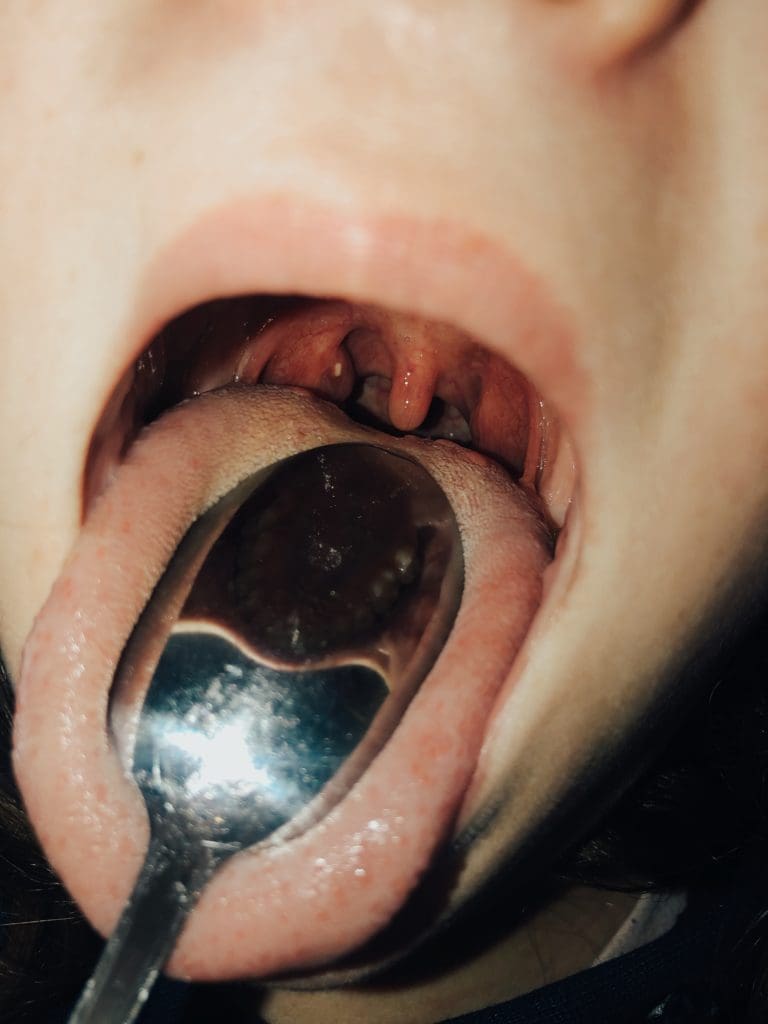
After showing this picture to her pediatric ENT, he said it was most likely a tonsil stone. What is a tonsil stone? It’s basically a little calcified mass of grossness, caused by bacteria in the mouth; the ENT told me that it’s believed to be caused by the same bacteria that causes tartar on teeth.
After talking over her symptoms, the ENT recommended that Sierra have a tonsillectomy, and surgery was scheduled for the following week.
Pre-Surgery Prep for a Tonsillectomy

Sierra wasn’t allowed to eat solid foods for at least 8 hours prior to our hospital check in, and she wasn’t allowed to drink for the last 3 hours before, either. Luckily, her surgery check in was scheduled for 8:00am so it made this part a lot easier for us! Originally she was scheduled for later in the afternoon so I was super grateful that there was a cancellation the day before so Sierra could get an earlier time slot.
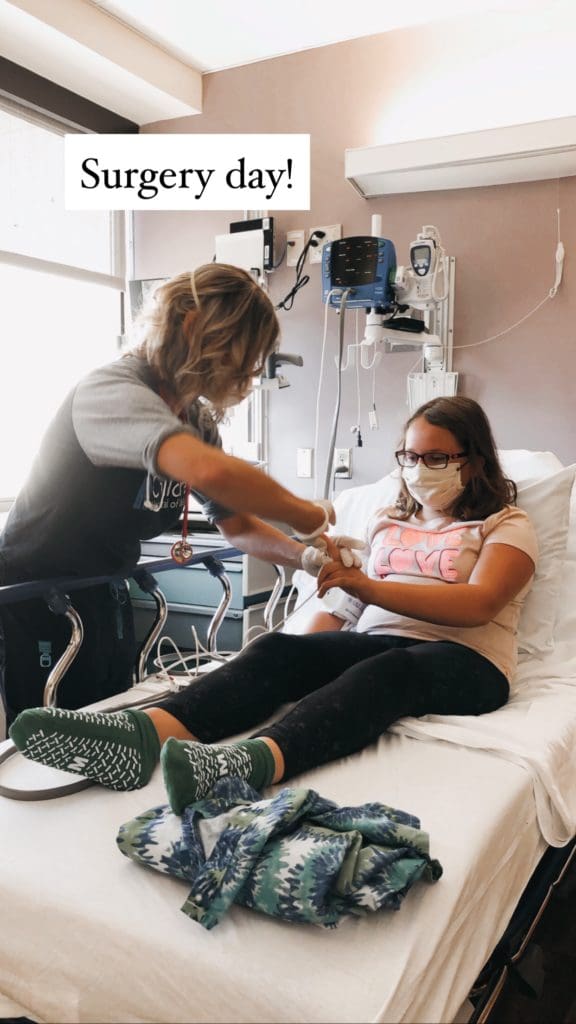
Once we arrived at the hospital, Sierra was taken back for a bunch of pre-op work. The nurse took her blood pressure and pulse, and she made her feel as calm and comfortable as possible.
After Sierra got changed into her hospital gown, her ENT came in to talk with us and answer all of our questions. He also took the time to reassure Sierra, and even though she was super nervous, she got to ask questions and he answered them for her.
After the surgeon came in, the anesthesiologist came in to talk with us. She was amazing, too; reminded me of a sweet older auntie, who was there to take care of my daughter. She answered all of our questions, and took the time to reassure Sierra.
It took about an hour and a half or so to get checked in and meet with the ENT and anesthesiologist. About 20 minutes before the surgical team came to whisk her into the operating room, Sierra’s pre-op nurse came in with some “silly syrup” and boy did it make her silly. It took about 10 minutes to kick in, but once it did? Oh boy. 😂
The “laughing liquid” had a dual purpose: first, it made her anxiety evaporate. She was full of giggles and not afraid, even when the surgical team came to take her to the OR. Second, it had an analgesic effect making it so she wouldn’t remember leaving us or going to the OR.
Then it came time to wait. 😬
She was away from us for about an hour. We ran (literally) to the Starbucks downstairs to get some coffee, and then sat in the waiting room staring at the surgical update board.

Finally!!!! We got pulled into a private room for the surgeon to meet up with us, to let us know how it went. I’ll be honest, getting pulled into a room “for privacy” and the receptionist not being allowed to tell us whether or not she was okay was the least awesome part of our experience. Maybe I watch too much TV and let my anxiety get the best of me, but, I didn’t appreciate it; especially since we had to sit and wait for like 10 minutes in the room by ourselves.
Once the surgeon came in, he told us that everything went great (phew!). He said it was a “nice and boring” surgery, which was exactly what we wanted. He did mention, however, that a “ton of debris came spilling out” when he removed her tonsils, which about made me want to puke right there in that little room. After we had a chat, we were sent back out into the waiting room so we could join Sierra in recovery.
Tonsillectomy Recovery in the Hospital
This was honestly the worst part for me as a mom. When we were escorted back to recovery, I could hear Sierra panicking and crying from down the hall. She woke up quickly from anesthesia but she was absolutely beside herself – she couldn’t talk, she kept rocking back and forth and shaking her head, she couldn’t breathe well and she was trying to talk but couldn’t because she was slurring her words. It took everything in me not to seriously break down in tears when I was trying to get her to calm down.
I gave the nurse more than one panicked look, and she reassured me that this type of reaction was expected and common. So while it is scary to someone who has never seen it before, there was nothing to be alarmed about.
Finally after several minutes of being with her in the initial recovery room, she was approved to go back to her second recovery room. The nurse tried to put a mask on her and I went a little momma bear on her; Sierra had to get a covid test the day before surgery (which came back negative, obviously) and I got furious that that they tried to mask her unnecessarily when she was already agitated. The nurse obliged and asked Sierra to pull her sheet over her face 🙄 which she did for about 4 seconds on the walk down the hallway.
It took almost an hour for Sierra to calm down, and start to eat popsicles and apple sauce. We spent the next couple of hours keeping her from getting too agitated, getting her drink and have ice cream. Sierra’s new recovery nurse was amazing and really helped Sierra calm down, kept her hydrated and brought all her favorite ice cream flavors.
Finally, after six hours in the hospital, Sierra was discharged!
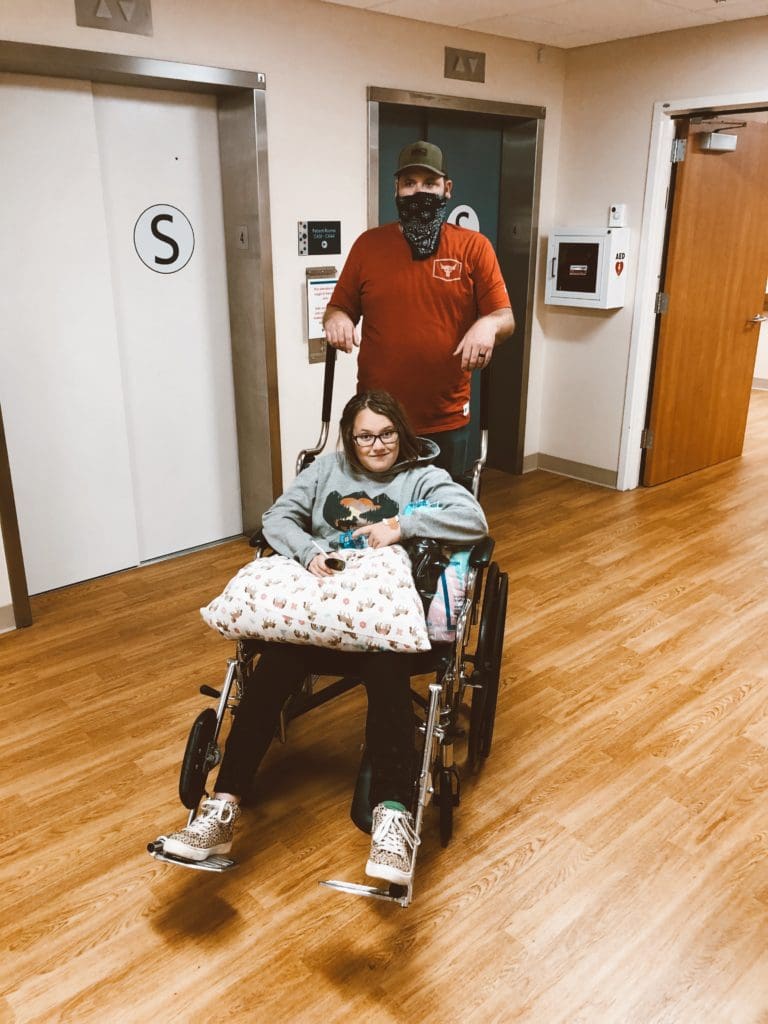
The First Few Days After a Tonsillectomy
The worst part for Sierra has been how hungry she has been, but not being able to really eat. Her stomach has been aching, and after 3 days of popsicles, ice cream and protein shakes, all she wants is some real freaking food. Her tongue and throat got pretty swollen the next day, but the worst days for pain so far has been days 3 and 4.
The surgeon prescribed her Tylenol, Motrin and Oxycontin for pain management. I was really nervous about Sierra taking such a strong and possibly addictive medication 😬 but I’m glad she had it available, especially the last couple of days . There were a couple points where the Tylenol and Motrin couldn’t take the edge off, and she ended up in hysterics from the pain.
On Day 5, Sierra’s tonsils are nasty gross looking but I am told that they look exactly how they’re meant to look at this stage of recovery.
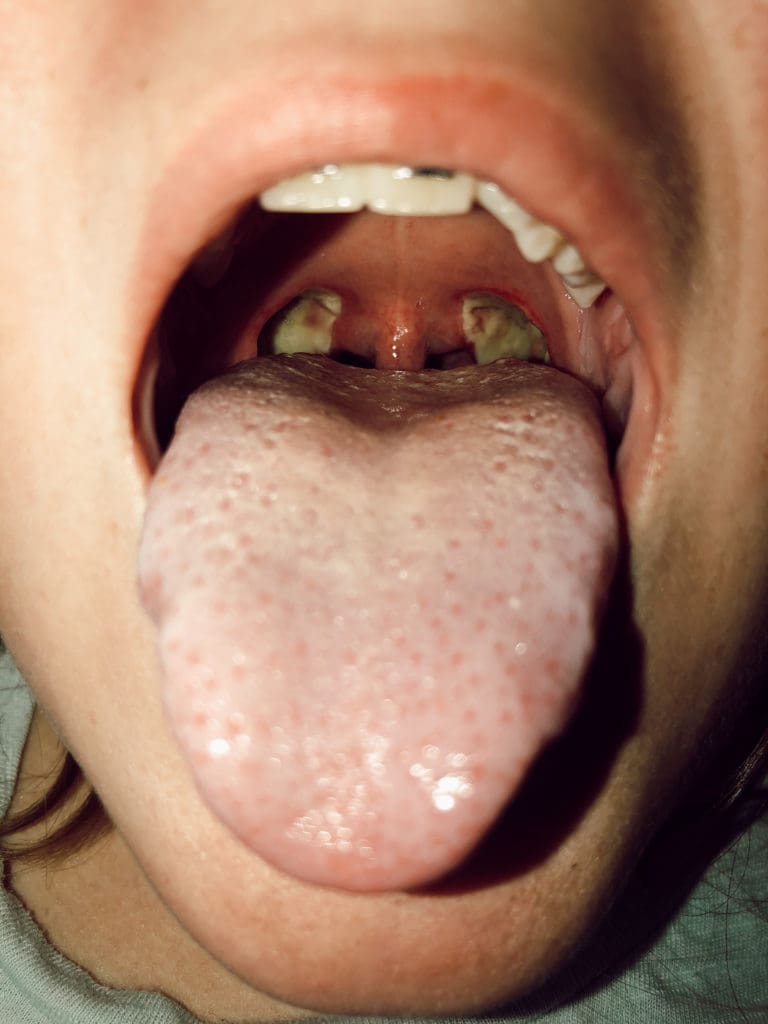
What to Expect When Your Teenager Has a Tonsillectomy
Here are a few things that parents might expect when their teenager has a tonsillectomy. These were things we either assumed or didn’t know to expect!
1.) They might not be sleepy. We expected Sierra to totally sleep away the rest of the first day after surgery, but she didn’t even nap. Not even on our hour-long car ride home from the hospital!
2.) They are going to be starving. Sierra’s chief complaint, aside from the pain, was how hungry she is. I never thought I’d hear her say “I hate ice cream” but here we are on day 5, and she hates popsicles and ice cream. We have no less than 8 different types of ice cream and popsicles in all kinds of forms and flavors and she’s at the point where she thinks they’re all gross.
3.) Referred pain is real. Sierra’s ears and jaws have been the most painful part of the recovery process, to the point of punching pillows and wailing. The term “referred pain” means that pain is sometimes felt in areas not actually affected by surgery, usually something in close proximity (i.e. ears to the throat).
4.) Staying on top of pain medication is absolutely necessary. Sierra is alternating 2 main medications (ibuprofen and acetaminophen) every 3 hours and has a third (Oxycontin) as a backup pain reliever taken as needed (no more than every 6 hours). She has woken up in the middle of the night in pain every single night since her surgery, especially if she misses a 3 hour dose. Last night was the worst, because of the referred pain in her ears.
I’ve read that this can last up to 10 days after surgery and I’ll tell you what: I don’t look forward to bedtime right now because I know she’s going to wake up in the middle of the night in tears. So if your teenager has a tonsillectomy – be sure you’re helping them keep track of their medications!

Big Thanks
I would be remiss if I didn’t give a big thanks to the surgical team at Children’s Hospital of Wisconsin in Milwaukee. Everyone made our experience as smooth as possible, and the entire team did an excellent job at keeping Sierra (and us parents!) very calm, informed and supported during this experience.
+ view comments . . .